 Alternatives to amalgam include composite resin, glass ionomer, porcelain, and gold, among other options. Most consumers choose direct composite fillings because the white coloring matches the tooth better and the cost is considered moderate.
Alternatives to amalgam include composite resin, glass ionomer, porcelain, and gold, among other options. Most consumers choose direct composite fillings because the white coloring matches the tooth better and the cost is considered moderate.
In the past, a common argument against composite fillings was that they were not as durable as amalgam. However, recent studies have debunked this claim. Researchers of a study which was published in 2016 and conducted on over 76,000 patients for over ten years found that posterior amalgam fillings had a higher annual failure rate than composites.1Two separate studies published in 2013 found that composite fillings performed as well as amalgam when comparing failure rates2and replacement filling rates.3Other research has offered similar findings: a study published in 2015 documented “good clinical performance” of composite resins over a 30-year evaluation,4a meta-analysis published in 2014 noted “good survival” of posterior resin composite restorations,5a study published in 2012 showed certain types of composite materials last as long as amalgam,6and a study published in 2011 found “good clinical performance” of composites over a 22-year period.7
Composite fillings have also been criticized because some of them contain the controversial material bisphenol-A (BPA). Dentists have a variety of opinions about the safety of BPA and other types of bisphenol, such as Bis-GMA and Bis-DMA. There has likewise been concern about glass ionomers, all of which contain fluoride.
Patients who are concerned about the ingredients in their dental materials often choose to speak with their dentists about using a material that does not contain certain ingredients. For example, a product named Admira Fusion8/Admira Fusion X-tra9released in January 2016 by the dental company VOCO is reported to be ceramic10and not to contain Bis-GMA or BPA before or after it has been cured.
Another option for dental patients concerned about which mercury-free alternative to use as a filling material is to do their own research and/or take a dental biocompatibility test. If biological testing is used, a patient’s blood sample is sent to a laboratory where the serum is evaluated for the presence of IgG and IgM antibodies to the chemical ingredients used in dental products.11 The patient is then provided with a detailed list of which name-brand dental materials are safe for their use and which ones could result in a reaction. Two examples of labs that currently offer this service are Biocomp Laboratories12and ELISA/ACT Biotechnologies13
Also, in regard to dental allergies, Dr. Stejskal introduced the MELISA test in 1994. This is a modified version of the (Lymphocyte Transformation Test) LLT designed to test for metal sensitivity type IV delayed hypersensitivity to metals, including sensitivity to mercury.14
In addition to considering which material to use for dental fillings, it is essential that dental patients and professionals be familiar with and utilize safety measures when removing dental amalgam mercury fillings.
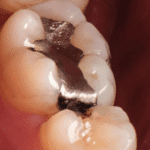
Dental amalgam danger exists because mercury fillings are associated with a number of human health risks.

Learn about steps that can be taken to protect patients, dentists, and environment during dental amalgam mercury removal.

This thorough document includes an extensive bibliography on the subject of dental mercury in the form of over 900 citations.


