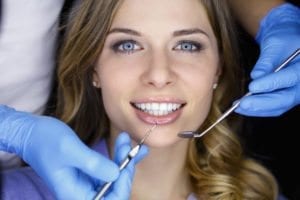
IAOMT promotes oral health integration
While periodontal disease is accepted by the medical community for its role in cardiovascular problems and diabetes, the effects of other dental conditions and materials on whole body health have yet to be extensively recognized. However, since the mouth is the gateway to the digestive tract, it should not be surprising that what happens in the oral cavity impacts the rest of the body (and vice versa, as in the case of diabetes). Although it might seem obvious that dental conditions and materials can influence the entire human system, there is a clear need for the mainstream medical community, policy makers, and the public to be educated about this reality.
Biological Dentistry and Oral Health Integration
Biological dentistry is not a separate specialty of dentistry, but a thought process and an attitude that can apply to all facets of dental practice and to health care in general: to always seek the safest, least toxic way to accomplish the goals of modern dentistry and of contemporary health care and to recognize the essential connections between oral health and overall health. The tenets of biological dentistry can inform and intersect with all topics of conversation in health care, as the well-being of the mouth is an integral part of the health of the whole person.
Biological dentists encourage the practice of mercury-free and mercury-safe dentistry and aim to help others understand what these terms actually mean in clinical application:
- “Mercury-free” is a term with a wide-range of implications, but it typically refers to dental practices that do not place dental mercury amalgam fillings.
- “Mercury-safe” typically refers to dental practices that use innovative and rigorous safety measures based on up-to-date scientific research to limit exposure, such as in the case of removing previously existing dental mercury amalgam fillings and replacing them with non-mercury alternatives.
- “Biological” or “Biocompatible” dentistry typically refers to dental practices that utilize mercury-free and mercury-safe dentistry while also considering the impact of dental conditions, devices, and treatments on oral and systemic health, including the biocompatibility of dental materials and techniques.
In addition to consideration for the risks of mercury fillings and biocompatibility of dental materials (including the utilization of allergy and sensitivity testing), biological dentistry further addresses heavy metals detoxification and chelation, nutrition and oral cavity health, oral galvanism, risks of topical and systemic fluoride exposure, the benefits of biological periodontal therapy, the influence of root canal treatments on patient health, and the diagnosis and treatment of neuralgia inducing cavitational osteonecrosis (NICO) and jawbone osteonecrosis (JON).
Within our membership, IAOMT dentists have varying levels of training in mercury-free, mercury-safe, and biological dentistry. Click here to learn more about biological dentistry.
Evidence of Need for Oral Health Integration
A number of recent reports have clearly established the urgency for oral health to be better integrated into public health. In fact, Healthy People 2020, a project of the U.S. government’s Office of Disease Prevention and Health Promotion, has identified a key area of public health improvement: to increase awareness of the importance of oral health to overall health and well-being.1
One reason for this needed awareness is that millions of Americans have dental caries, periodontal disease, sleep disordered breathing issues, cleft lip and palate, oral and facial pain, and oral and pharyngeal cancers.2 The potential consequences of these oral conditions are far-ranging. For example, periodontal disease is a risk factor for diabetes, heart disease, respiratory disease, stroke, premature births, and low birth weights.3 4 5 Additionally, oral health problems in children can lead to attention deficits, difficulty in school, and dietary and sleep issues.6 Also, oral health problems in older adults can lead to disability and reduction in mobility.7 These are only a few examples of the known repercussions of impaired oral health on overall health.
In their 2011 report Advancing Oral Health in America, the Institute of Medicine (IOM) made the necessity of inter-professional health collaboration clear. In addition to improving patient care, the integration of oral health with other disciplines was recognized as a means of reducing health care costs.8 Further, the IOM warned that the separation of dental professionals from other health care professionals negatively influences patients’ health.9 More precisely, Chairman of the Committee on Oral Health Initiative Richard Krugman stated: “The oral health system still largely depends on a traditional, isolated dental care model in the private practice setting—a model that does not always serve significant portions of the American population well.”10
The reality of patients enduring harmful consequences as a result of oral health being excluded from medical programming has been confirmed in other reports. In a commentary published in the American Journal of Public Health, Leonard A. Cohen, DDS, MPH, MS, explained that patients suffer when there is no connection between the dentist and physician.11 Interestingly, it has been reported that patients want this connection to made, as researchers have noted: “As interest in integrative health care and the use of complementary and alternative therapies by consumers has continued to grow, concern has increased that health professionals be sufficiently informed about integrative health so that they can effectively care for patients.”12
It is obvious that patients and practitioners mutually benefit from an integrated approach to oral health and public health. First, oral health conditions can be indicative of other health problems including nutritional deficiencies, systemic diseases, microbial infections, immune disorders, injuries, and some forms of cancer.13 Next, patients enduring adverse symptoms from oral health conditions such as infections, chemical sensitivities, TMJ (temporomandibular joint disorders), craniofacial pain, and sleep disorders can benefit from inter-professional collaboration. Such collaboration has also been called for in regard to oral complications from cancer treatments and other medications14 and in regards to biocompatible materials.15 Biocompatibility is especially crucial because dental mercury allergies can result in an array of subjective and objective health complaints16 and impact as many as 21 million Americans today.17 However, these figures could be even higher because recent studies and reports suggest that metal allergies are on the rise.18 19
Essential Improvements for Oral Health Integration
All of these circumstances and more provide evidence that oral health issues must become more prevalent in medical education and training. Because dental schools and education are completely separate from medical schools and continuing education, physicians, nurses, and other health care professionals are often not knowledgeable about oral health care, including recognition of oral diseases.20 In fact, it has been reported that only 1-2 hours per year of family medicine programs are allotted for dental health education.21
The lack of education and training has wide-ranging implications for public health. In addition to all of the conditions and scenarios mentioned above, other consequences might not be as obvious. For instance, most patients with dental complaints seen by hospital emergency departments (ED) are usually suffering from pain and infection, and the lack of ED knowledge about oral health has been cited as a contributor to opiate dependency and antibiotic resistance.22
This lack of awareness appears to be due to lack of opportunity. While practitioners have demonstrated interest and training about oral health, this topic has traditionally not been offered in medical school curricula.23 However, changes have been encouraged, such as Chairman of the Committee on Oral Health Initiative Richard Krugman’s advice: “More needs to be done to support the education and training of all health care professionals in oral health care and to promote interdisciplinary, team-based approaches.24
The encouragement for such urgent changes appears to be having an effect. Some innovative examples of existing models and frameworks are forging a new future in the integration of oral and public health. The IAOMT is part of this new future and promotes active cooperation between dentists and other health professionals so that patients can experience a more optimum level of health.